
At the office of Erin A. Fontenot, DDS, our priority is straightforward: protect your oral health with care that’s precise, comfortable, and respectful. When preservation of a tooth isn’t possible or would compromise nearby structures, extraction becomes a thoughtful, deliberate step toward a healthier mouth. We focus on clear explanations so you understand the reasons behind any recommendation and the options that follow.
Tooth removal is never the first choice, but it can be the most responsible one when the long-term outcome is considered. Removing a problematic tooth can stop infection, address pain, prevent damage to adjacent teeth, and set the stage for restorative solutions that preserve function and appearance. Our team treats each case individually and tailors care to your needs and medical history.
Below you’ll find a practical look at common situations that lead to extraction, how we evaluate and plan treatment, what to expect during different procedures, and straightforward guidance for recovery and next steps. The information is intended to help you make informed decisions and feel confident about your care.
Persisting baby teeth that interfere with development
Sometimes a primary tooth remains firmly in place and blocks the eruption of the permanent tooth beneath it. When a baby tooth fails to resorb or becomes fused to the jawbone, extraction can help the permanent tooth erupt properly and prevent alignment problems as your child grows.
Severe decay that has destroyed the tooth structure
Decay progresses from the outer enamel inward, and if it reaches a point where the tooth cannot be rebuilt reliably, removal may be the safest option. Extracting a non-restorable tooth prevents ongoing infection and damage to adjacent teeth and tissues.
Extensive fractures or structural failure
Teeth with complex vertical fractures, root damage, or significant loss of supportive structure sometimes cannot be saved. When a tooth is compromised beyond repair, extraction prevents future pain and helps maintain the health of surrounding teeth.
Advanced periodontal disease that weakens support
When gum disease destroys the tissues and bone that hold a tooth in place, loosening and infection can follow. In advanced cases where support cannot be restored predictably, extraction may be necessary to protect overall oral health.
Problematic wisdom teeth
Third molars often emerge late and may be poorly aligned, partially erupted, or prone to decay. If wisdom teeth threaten nearby teeth, cause recurrent infections, or create bite problems, removing them can prevent future complications.
Creating space for orthodontic treatment
In certain orthodontic plans, removing one or more permanent teeth is the most predictable way to create the necessary space for optimal alignment and a stable bite. These decisions are made in close collaboration with your orthodontic team to support long-term results.
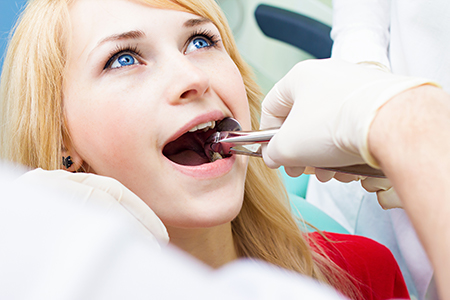
Before any extraction, we perform a thorough intake that goes beyond the immediate tooth. This includes reviewing your general health, medications, allergies, and any conditions that could affect healing. Understanding your whole-body health helps us identify precautions and coordinate care with your physician when necessary.
We routinely use clinical exams and digital radiographs to map the tooth’s roots, nearby nerves, and bone. These images help us choose the least invasive approach and anticipate challenges—such as curved roots, proximity to sinuses, or impacted teeth—that could influence whether a simple or surgical extraction is the best route.
If you take medications that affect bleeding or healing, or if you have a history of certain heart or immune conditions, we’ll discuss specific instructions to keep the procedure safe. We’ll also review sedation options if you feel anxious or need additional comfort during the appointment.
Not every tooth removal is the same. A simple extraction applies when the tooth is fully visible in the mouth and has a straightforward root shape. After numbing the area thoroughly with a local anesthetic, the dentist gently loosens the tooth and removes it with forceps. We take time to keep you comfortable and explain each step so you feel informed throughout the process.
Simple extractions are efficient and predictable. They typically require only local anesthesia and minimal healing time. For patients who prefer extra reassurance, we offer additional relaxation options to reduce stress during the procedure. After the tooth is removed, we’ll go over immediate care steps and what to expect in the first 24–72 hours.
Even with a simple extraction, our team monitors healing and provides clear instructions to reduce the risk of complications. We will also discuss whether and when tooth replacement should be considered to restore chewing function and prevent shifting of neighboring teeth.
Surgical extractions are indicated for teeth that are broken at the gum line, impacted, or fused to the bone. These procedures can require a small incision, removal of a bit of bone, or sectioning the tooth into pieces to remove it safely. A surgical approach gives better access and helps protect surrounding structures during removal.
For more complex cases, we may refer you to an oral and maxillofacial surgeon with specialized training. Regardless of who performs the procedure, you’ll receive individualized preoperative guidance and a clear plan for anesthesia and post-operative care to ensure the best possible outcome.
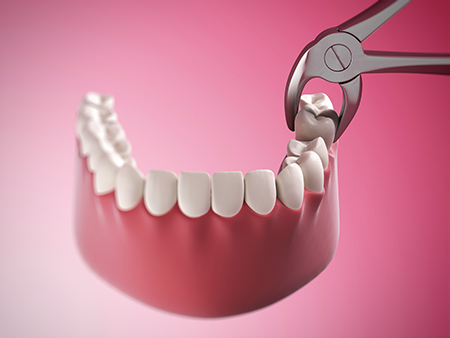
Healing after an extraction is a process the body performs naturally, and our role is to support that process with practical care instructions. We provide specific directions tailored to the complexity of the extraction, your medical situation, and any medications you are taking, so you know exactly how to care for the site in the days that follow.
Common short-term issues include mild bleeding, swelling, and soreness. These are usually manageable with gauze, rest, ice, and appropriate pain control. It’s important to follow the guidance provided so a stable blood clot can form and protect the site—this clot is a key part of normal healing.
Control bleeding with gentle pressure
We’ll place gauze over the extraction site; keep steady pressure as instructed until bleeding slows. Replace the gauze as needed, and contact the office if bleeding is excessive or persistent beyond the expected timeframe.
Protect numb tissues
Avoid chewing, sucking, or touching the area while anesthesia is in effect to prevent accidental bites or injury to your lips, cheeks, or tongue.
Take medications as directed
If antibiotics are prescribed, complete the full course. For pain, start with recommended over-the-counter options unless a prescription is given; taking analgesics early can make pain easier to manage.
Protect the clot and avoid suction
Do not rinse vigorously, spit forcefully, drink through a straw, or smoke for the first several days. These actions can dislodge the clot and slow healing.
Manage swelling
Apply ice to the face in short intervals on the day of surgery to reduce swelling. Keep your head elevated and avoid strenuous activity for the first 48 hours.
Eat soft, nourishing foods
Choose lukewarm, soft foods and stay well hydrated. Avoid hot, spicy, or carbonated beverages at first. Gradually return to your regular diet as comfort and healing allow.
Practice gentle oral hygiene
Brush nearby teeth carefully and, when advised, rinse gently with a mild saltwater solution to keep the area clean without disturbing the clot.
Follow-up appointments
If sutures were placed or your extraction was complex, we will schedule a follow-up visit to monitor healing. Be sure to attend any recommended appointments so we can check your progress and address concerns promptly.
If you notice increasing pain, worsening swelling, prolonged bleeding, or any unusual symptoms, contact our office so we can evaluate and advise the next steps.
When an extraction is necessary, the skill and judgment of your dental team matter. Our approach emphasizes careful diagnosis, clear communication, and gentle technique to minimize discomfort and support predictable healing. We coordinate with specialists and primary care providers when complex medical issues are involved.
After an extraction, we’ll review replacement options if needed—such as removable dentures, fixed bridges, or dental implants—and help you understand the timing and benefits of each approach. Our goal is to restore comfort and function while protecting the health of the entire mouth.
Whether you need a routine removal or a more complex surgical extraction, you can expect thoughtful planning and compassionate care from start to finish. Contact us for more information about extraction procedures and how we can help you or a family member move forward with confidence.
The most common reasons for tooth loss include advanced periodontal disease, extensive tooth decay, and facial trauma. According to statistics, gum disease is responsible for close to 70% of tooth loss in adults. Although less frequent than the preceding three reasons, it should also be noted that specific diseases, drugs, smoking, and poor nutrition contribute to the risk of tooth loss.
The Centers for Disease Control and Prevention report that in the United States, an average of 12 teeth (including the wisdom teeth) are lost by the age of 50. Also, 26% of adults between 65 and 74 years of age have lost all their teeth.
Every patient and every situation is different. However, when a tooth and the surrounding tissues are numbed with a local anesthetic, you should only expect to feel a bit of pressure, but no pain as the tooth is being loosened from the surrounding tissues and extracted. For patients who are apprehensive and for some surgical extractions, our office will discuss our options in dental sedation to provide further relaxation and reduce any sense of discomfort.
While it's normal to feel some tenderness and swelling following an extraction, the degree of these sensations can vary. It mostly depends on the complexity of the extraction and the body's response to the procedure. We'll recommend or prescribe the appropriate pain medication to help ensure your comfort and give you specific instructions for maximum effectiveness and safety.
Typically, the recovery period following a simple extraction is shorter than a surgical extraction. However, a patient's overall health, habits, the size and location of the tooth, and other variables can influence recovery and healing. To speed up the recovery and avoid any complications, patients must follow the given at-home instructions diligently. We'll carefully review what to expect following your procedure and go over your post-op instructions.
Smoking interferes with blood clot formation, which is an essential first step in the healing process. Blood clot formation not only provides a protective layer to cover the underlying exposed bone and nerve endings, but it also supports the growth of new tissue. Cigarette smoke also contains chemical toxins that can disrupt the healing process and lead to problems such as continued inflammation, infection, or dry socket.
In a very small percentage of cases, a condition known as dry socket can develop in the aftermath of a dental extraction. This painful condition can arise when the blood clot in the extraction site doesn't form properly or gets dislodged. With dry socket, you may experience throbbing pain and symptoms such as bad breath and an unpleasant taste in your mouth. As skilled providers of care, our office will provide immediate treatment to alleviate your discomfort and promote healing.
The last teeth in your mouth to develop, wisdom teeth often do not have enough room to fully erupt or may be positioned in the wrong direction. These issues can affect your dental health as well as overall wellbeing. While some individuals never develop all their wisdom teeth, and a few have sufficient space for them, there are many people with partially or fully impacted third molars. Our office will monitor the development, position, and health of your wisdom teeth and will advise you if and when extractions are indicated.
After a tooth is removed, bone-grafting material is sometimes placed in the socket to promote healing and encourage new bone development. This procedure is often performed to support the eventual and successful placement of a dental implant.
At the office of Erin A. Fontenot, DDS, we strive to make dental care affordable and accessible. Depending on the type or complexity of the extraction and other variables, the cost of the procedure can vary. Based on our diagnostic findings, our office will inform you of the healthiest choices in care, explain the fees, discuss insurance coverage, and explain your payment options.
Many dental plans offer some level of coverage for tooth extractions. We'll advise you if your plan covers the full cost of the procedure and if there is any out-of-pocket expense. Our business office will work with you to maximize your insurance benefits as much as possible while helping you minimize any out-of-pocket expenses.
Teeth may require extraction for several clinical reasons, including severe decay that has destroyed the tooth structure, extensive fractures that make restoration unpredictable, or advanced periodontal disease that has compromised supporting bone and gum tissue. Persistent primary teeth that block eruption of permanent teeth and orthodontic space needs can also lead to planned removals. Impacted or problematic wisdom teeth are a frequent reason for extraction when they threaten adjacent teeth or cause recurrent infection.
Extraction is typically considered only after evaluating restorative options and long-term prognosis for the tooth. Removing a non-restorable or harmful tooth can stop infection, eliminate pain, and protect neighboring teeth and tissues. The decision is individualized based on clinical findings, imaging, and your overall health status.
We begin with a thorough clinical exam and digital radiographs to assess the extent of decay, root configuration, bone support, and proximity to vital structures such as nerves and sinuses. Medical history, medications, and previous dental treatments are reviewed because systemic factors can influence healing and the safety of preserving a tooth. Sometimes additional testing or consultations with specialists help clarify whether predictable restoration is possible.
When the tooth cannot be reliably restored or poses a risk to adjacent teeth, extraction becomes the most responsible treatment choice. The team will explain the rationale, review possible alternatives, and outline next steps for replacement if needed. Clear communication ensures you understand the expected outcomes and the plan for follow-up care.
A simple extraction is performed on a tooth that is fully visible in the mouth and has a straightforward root shape; it typically requires only local anesthesia and forceps to loosen and remove the tooth. These procedures are often quick and have predictable healing with minimal intervention. A surgical extraction is more complex and is used when a tooth is broken at the gum line, impacted, or fused to bone.
Surgical extractions may involve a small incision, removal of a bit of bone, or sectioning the tooth into pieces to allow safe removal while protecting surrounding structures. Because they are more involved, surgical extractions may require sutures and a longer recovery period. For particularly complex cases, we may coordinate care with an oral and maxillofacial surgeon to ensure the best outcome.
Local anesthesia is the standard of care to numb the area and provide pain-free treatment during most extractions. For patients who experience dental anxiety or for more complex surgical procedures, additional options such as oral sedatives, nitrous oxide (laughing gas), or monitored intravenous sedation may be offered to enhance comfort and relaxation. The choice depends on the procedure complexity, medical history, and patient preference.
Before any sedation, we review your health history and provide specific preoperative instructions to ensure safety. Our team monitors vital signs during treatment and provides clear post-op guidance to support recovery. We will always discuss the recommended anesthesia plan and answer questions so you feel comfortable with the approach.
Preparation begins with sharing a complete medical history, including current medications, allergies, and any recent changes in health, so the team can identify risks and coordinate care with your physician if needed. Follow any preoperative instructions regarding fasting or medication adjustments, particularly if you will receive sedation or have a condition that affects bleeding or healing. Arrange for a responsible adult to accompany you if you expect sedation or have difficulty with mobility.
Wear comfortable clothing and plan for a period of rest after the procedure, especially following surgical extractions. Bring a list of medications and any pertinent medical documentation to the appointment to streamline care. If you have questions about specific preparations, the office staff can provide tailored guidance based on your situation.
During the first 24 to 72 hours, it is normal to experience mild bleeding, swelling, and soreness at the extraction site; these symptoms are part of the body’s healing response and typically improve each day. You will be advised to apply ice intermittently on the day of surgery, rest with your head elevated, and avoid activities that increase blood pressure or dislodge the clot, such as heavy exercise or vigorous rinsing. Pain can usually be managed with recommended analgesics taken as directed and by following the care instructions provided.
Maintain gentle oral hygiene around the area and stick to soft, lukewarm foods while the site stabilizes. Avoid smoking, using straws, or forceful spitting, as these actions can interfere with clot formation and healing. If you notice increasing pain, persistent bleeding, fever, or other concerning signs, contact the office promptly for evaluation.
Dry socket occurs when the blood clot protecting the extraction site is dislodged or fails to form, exposing underlying bone and nerve endings and causing increased pain. To reduce this risk, follow post-op instructions carefully: avoid smoking, do not use straws, refrain from vigorous rinsing or spitting, and limit physical exertion for the first several days. Gentle rinsing with a mild saltwater solution is usually recommended only after the initial 24 hours and should be done softly to avoid disturbing the clot.
Taking prescribed or recommended medications as directed, attending follow-up appointments, and maintaining careful oral hygiene around the surgical site help support predictable healing. If you have conditions or medications that affect healing, notify the team so we can implement additional precautions. Prompt communication about unusual pain or drainage enables timely treatment to prevent more serious complications.
Wisdom teeth are often removed when they erupt partially or are misaligned, which can create pockets that trap bacteria and food, leading to recurrent infection, decay, or gum disease. Impacted wisdom teeth that press on adjacent teeth, cause crowding, or threaten the health of neighboring roots are commonly recommended for removal. In some cases, preemptive removal is advised to prevent future problems when monitoring suggests a high likelihood of complications.
The timing of removal depends on factors such as root development, position, symptoms, and the patient’s overall health. Young adults often experience fewer complications and faster recovery because bone is more pliable and roots are less fully formed. Decisions about extraction are based on clinical examination and imaging to weigh the potential benefits and risks for each individual.
Timing for tooth replacement depends on the extraction complexity, presence of infection, bone quality, and your overall health; immediate replacement is possible in some situations, while other cases benefit from a healing interval to allow bone and soft tissues to recover. Dental implants often require a staged approach where the socket is allowed to heal for a period of months before implant placement, unless conditions are favorable for immediate implantation. Fixed bridges or removable options can sometimes be used sooner to restore function and appearance during the healing phase.
We will review replacement options after evaluation of the extraction site and discuss the recommended timeline that best supports long-term success. Planning may include bone grafting or tissue management when necessary to optimize future restorative outcomes. For personalized guidance, the team will explain the advantages and timing considerations for implants, bridges, and removable prosthetics so you can make an informed choice.
Extractions for children often focus on preserving proper dental development and guiding eruption of permanent teeth; removing a problematic primary tooth can prevent crowding or misalignment and support normal growth. Pediatric considerations include the child’s emotional readiness, behavior management techniques, and the use of age-appropriate anesthesia or sedation when necessary. Clinicians also evaluate whether space maintenance or coordination with an orthodontist is needed following the extraction.
Parents should provide a complete medical history and follow pre- and post-operative instructions tailored to pediatric patients, including guidance on pain control, diet, and activity restrictions. The dental team aims to make the experience as calm and safe as possible, using clear communication and follow-up care to monitor healing and development. If concerns arise about speech, chewing, or eruption patterns after an extraction, timely evaluation helps address issues proactively.
