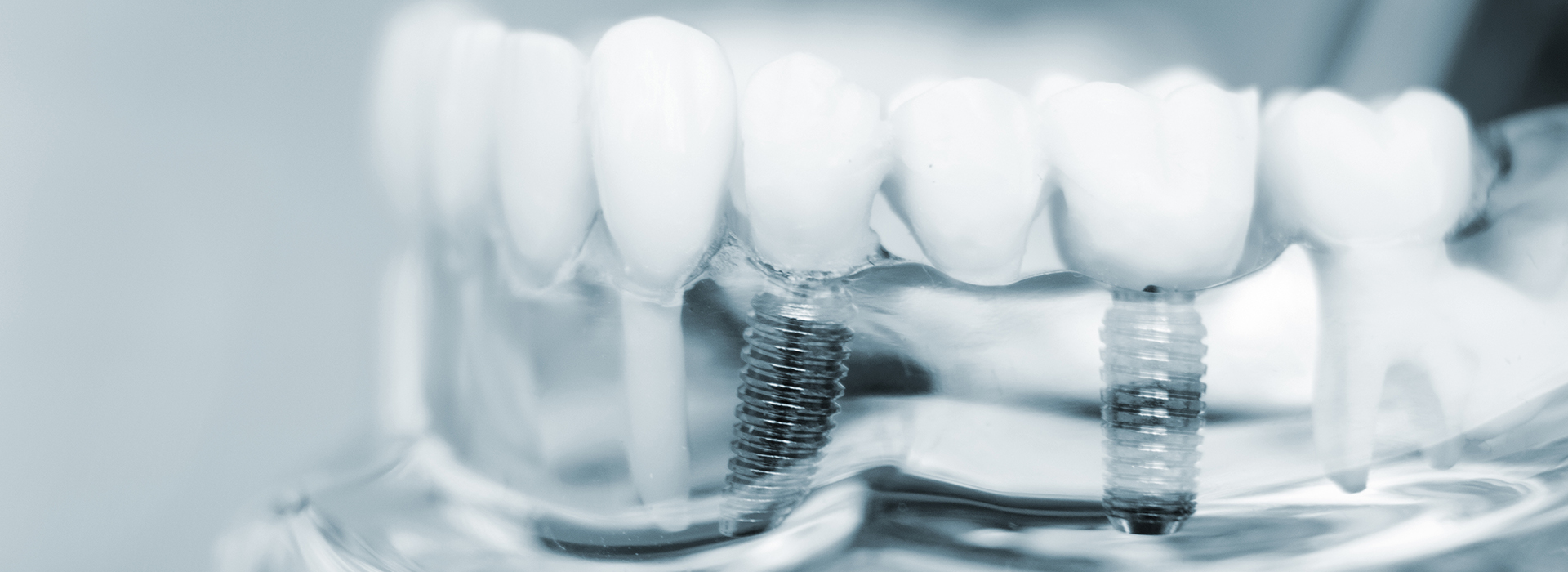
Tooth loss affects many people at different stages of life, and the consequences reach beyond aesthetics. Missing teeth can change how you chew, how you speak, and how your face ages over time. Modern implant dentistry focuses on restoring both function and form by replacing the full structure of a tooth — root and crown — rather than just the visible portion.
At the office of Erin A. Fontenot, DDS, we emphasize predictable, evidence-based care that helps patients regain comfortable, long-lasting function. Implants are engineered to integrate with the jawbone, offering a level of stability and performance that closely mirrors natural teeth. That stability translates into confidence during everyday activities like eating, laughing, and speaking.
Because implants address the underlying bone loss that often follows extraction or long-term tooth absence, they do more than fill a gap — they help preserve facial contours and support oral health over time. For many patients, that combination of durability and biology makes implants the most sensible option for restoring a healthy smile.

One of the defining advantages of dental implants is how closely they replicate a natural tooth’s performance. Unlike conventional removable dentures, an implant is anchored into the jawbone and can support crowns, bridges, or full arches without relying on adjacent teeth for stability. This root-like support allows for predictable chewing force and better preservation of bite mechanics.
From a cosmetic standpoint, implants let restorative teeth be designed with careful attention to color, shape, and proportion so they blend seamlessly with the rest of the smile. When fabricated and positioned precisely, implant restorations are subtle — often indistinguishable from the surrounding teeth to friends, family, and colleagues.
Another practical benefit is convenience: implant-supported restorations eliminate many of the daily adjustments and adhesives that some removable appliances require. The result is a restoration that feels more integrated with the mouth and demands routine oral hygiene similar to natural teeth.
Dental implants are biocompatible titanium or titanium-alloy posts designed to be placed into the jaw and accept a prosthetic tooth once healed. After placement, the implant goes through osseointegration — a process where bone gradually bonds to the implant surface. This biological connection creates a strong foundation for single crowns, multi-tooth bridges, or full-arch reconstructions.
Because implants transfer chewing forces down into the bone in a manner similar to natural tooth roots, they help preserve bone volume and reduce the long-term shrinkage that often follows tooth loss. That preservation matters not only for function but also for maintaining facial proportions and reducing the hollowed appearance that can accompany untreated tooth loss.
Implants also come in a variety of shapes and surface treatments to suit different clinical scenarios. Your treatment plan will recommend the type and size of implant that best supports the prosthesis and the surrounding anatomy, with the goal of maximizing long-term stability.
Traditional bridges and removable dentures remain valid options for many patients, but implants provide distinct advantages in several key areas. They deliver superior retention and stability, significantly reducing the chance of movement during speech or eating. That reliability improves comfort and expands dietary freedom, which matters for everyday quality of life.
Implants also protect neighboring teeth. A conventional bridge requires preparation of adjacent healthy teeth to support the replacement crowns; implants, by contrast, are standalone supports that preserve surrounding tooth structure. Over time, this can reduce the need for future restorative work on those adjacent teeth.
Durability is another factor. With appropriate planning, implant placement, and routine oral maintenance, implant restorations are designed for longevity. They resist decay in the implant itself and maintain function without the frequent relining or adjustments that some removable prostheses require.
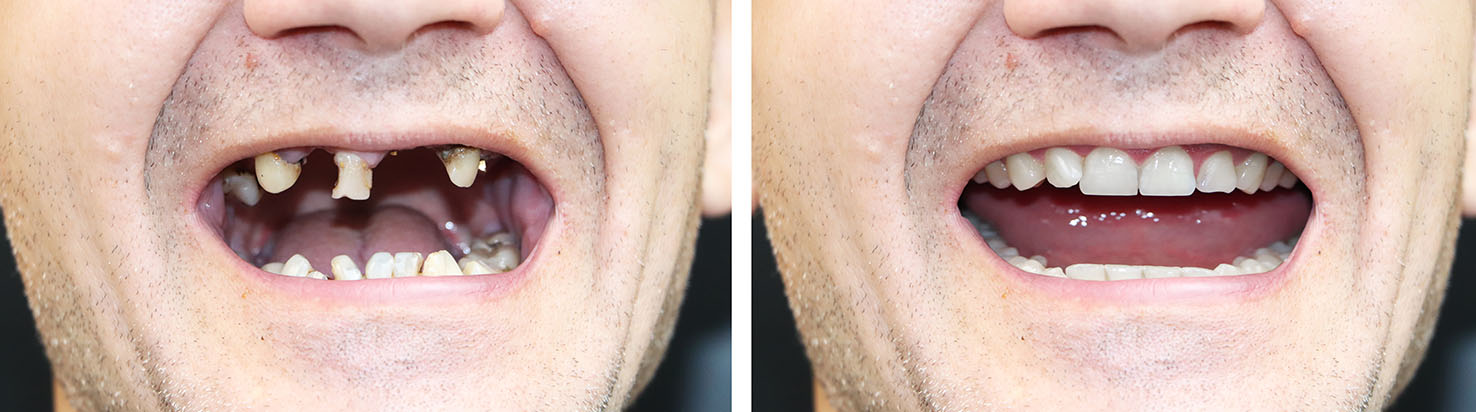
Determining candidacy for implants begins with a comprehensive evaluation of your medical and dental history, current oral health, and lifestyle. We consider factors such as gum health, bone volume, overall health status, and habits that can affect healing. Imaging and digital planning help create a clear picture and inform a personalized treatment map.
Not every patient follows the same timeline. Variables such as prior extractions, bone loss, or the need for additional procedures will influence sequencing and healing time. Our recommendations prioritize clinical predictability and long-term outcomes, balancing patient goals with sound surgical and prosthetic principles.
Implant surgery is typically performed in an outpatient setting and is well-tolerated with local anesthesia and optional sedation. The extent of the procedure depends on how many implants are needed and whether preparatory work — such as tooth extractions or grafting — is required. Patients generally experience minor discomfort that is manageable with prescribed aftercare and commonly resolves within days to weeks.
After placement, implants require time to integrate with the bone. In many cases a provisional restoration can restore appearance and basic function during healing, with the final prosthesis placed once osseointegration is confirmed. Throughout recovery we provide clear post-operative guidance and monitor healing closely to support a successful outcome.
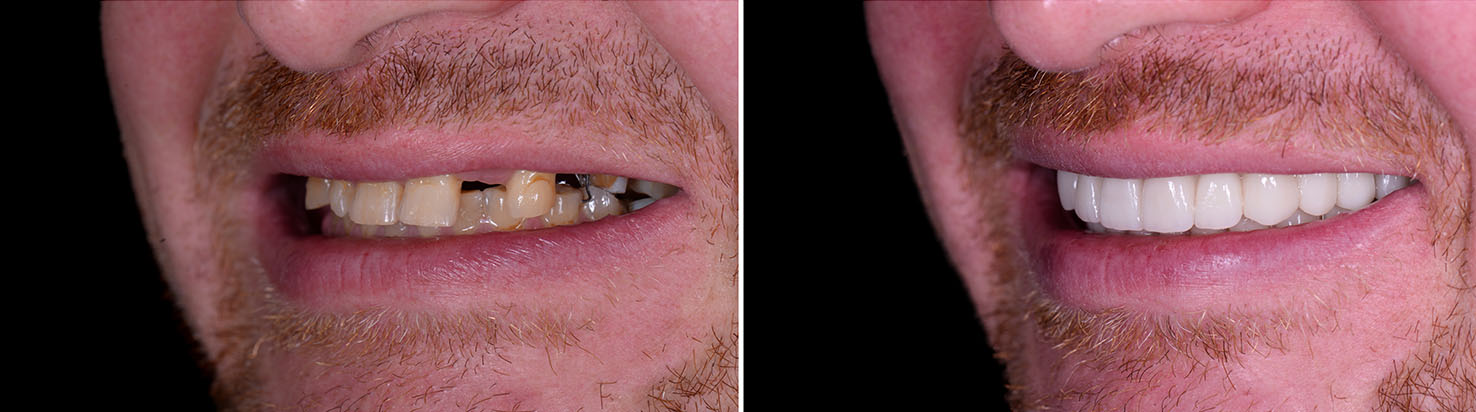
Implant success depends on sufficient bone to anchor the posts. If bone has been lost due to infection, long-term tooth absence, or injury, bone grafting can rebuild the site and create the volume needed for stable implant placement. Grafts can be placed at the time of extraction, prior to implant surgery, or simultaneously with implant placement depending on the situation.
There are several grafting techniques and materials available, and the choice is based on the amount of bone needed and the anticipated healing timeline. Bone grafting is a predictable adjunct to implant therapy and, when indicated, is an important step toward a durable, functional restoration.
Replacing missing teeth with implants is not just a cosmetic decision — it’s an investment in your oral function and overall wellness. Implants restore biting efficiency, stabilize the bite, and help maintain the jawbone and facial proportions that contribute to a natural appearance. Over time, these benefits support better nutrition, clearer speech, and greater confidence in everyday life.
If you’d like to learn more about implant dentistry and how it could apply to your smile, please contact us for additional information or to arrange a consultation. Our team is available to explain your options and guide you through each step toward a healthier, more resilient smile.
If you've lost a tooth due to injury, decay, gum disease, or any other reason, we recommend dental implants to replace missing teeth. Dental implants come the closest to replicating the look, feel, and function of your natural teeth.
Dental implants are placed into the jawbone and mirror the same function as the root of a tooth. The procedure for dental implants is usually performed while a patient is sedated. Patients who undergo IV sedation must have an empty stomach and transportation home following the procedure. Most sedation patients will have little to no memory of the procedure occurring.
Generally, dental implants are made out of a biocompatible metal such as titanium. Biocompatible metals are also used for other common bone implants (such as shoulder, hip, and knee replacements). The visible portion of the implant is usually made out of porcelain and is custom-made to match your existing teeth.
Dental implants are designed to fuse to the bone, which makes them become permanent fixtures. Typically speaking, the success rate is nearly 100%. There are few cases in which the implant will not fuse as intended and must be removed. If this happens to occur, the procedure can be attempted again a few months later.
Dental implants are not usually covered by dental insurance, but may be covered under a patient's medical insurance. Our office and your insurance company can discuss coverage options with you based on your individual case and treatment plan.
It's easy... just take care of an implant as if it's a natural tooth! This involves regular brushing, flossing, and dental checkups. If you have any concerns about your implant, contact us immediately.
Dental implants are small biocompatible posts, typically made of titanium or a titanium alloy, that are placed into the jaw to replace the root portion of a missing tooth. Once the implant is positioned, it provides a stable foundation for a custom prosthetic such as a crown, bridge, or full-arch restoration. By replacing both root and crown, implants restore chewing function and help maintain the structural relationships of the mouth.
Implant restorations are designed to mimic the form and function of natural teeth, allowing for predictable biting forces and improved comfort compared with many removable options. Because implants transfer chewing forces into the bone like a natural root, they support surrounding structures and contribute to long-term oral health. The result is a durable, discreet restoration that integrates with daily oral care routines.
After an implant is placed, the surrounding bone gradually bonds to its surface through a process called osseointegration. This biological connection creates a rigid, long-lasting attachment that allows the implant to support a prosthetic tooth much like a natural root supports a crown. The stability provided by osseointegration is essential for reliable chewing function and for preventing micro-movement that can compromise the restoration.
Because the implant transfers functional load into the jaw, it helps preserve bone volume and reduces the resorption that commonly follows tooth loss. Maintaining bone height and width supports facial contours, occlusal relationships, and the long-term success of adjacent restorations. Thoughtful implant selection and surgical technique enhance the chance of predictable integration and long-term stability.
Good candidates for dental implants generally have healthy gums, adequate jawbone volume or the willingness to undergo grafting when necessary, and overall medical conditions that support normal healing. Factors such as uncontrolled diabetes, active periodontal disease, heavy tobacco use, or certain medications can affect candidacy and should be discussed candidly during evaluation. Age alone is not a barrier; rather, biological health and local conditions guide the decision-making process.
For patients with reduced bone or other local challenges, predictable adjunctive procedures such as bone grafting or sinus augmentation can create the conditions needed for implant placement. The treatment plan is individualized based on imaging, clinical findings, and patient goals to balance function, esthetics, and long-term predictability. Collaborative planning with restorative and surgical considerations improves outcomes for a wide range of patients.
The evaluation begins with a thorough review of your medical and dental history, a clinical exam, and diagnostic imaging to assess bone anatomy and tissue health. Digital planning tools and three-dimensional imaging are often used to map implant position relative to nerves, sinuses, and adjacent teeth, enabling precise surgical guides and more predictable prosthetic outcomes. The team will discuss restorative options, timelines, and any preparatory procedures needed to optimize success.
At the office of Erin A. Fontenot, DDS, treatment planning emphasizes evidence-based sequencing and clear communication so patients understand each phase of care. Recommendations may include extractions, grafting, or temporary restorations to support healing and esthetics during integration. A customized plan outlines the expected number of visits, anticipated healing intervals, and the role of provisional appliances when appropriate.
Implant placement is typically performed in an outpatient setting using local anesthesia and, if desired, conscious sedation for comfort. The procedure involves positioning the implant into the prepared site in the jaw; the exact steps vary with the number of implants and whether additional procedures such as grafting are performed simultaneously. Many patients tolerate the procedure well and return home the same day with postoperative instructions and a short course of supportive care.
Initial healing generally takes a few weeks for soft tissues and several months for complete osseointegration, depending on the clinical situation. During this time a provisional prosthesis can often restore appearance and limited function. Follow-up visits monitor healing, manage any discomfort, and confirm readiness for the final prosthesis once integration and tissue health are assured.
Bone grafting is recommended when the jaw lacks sufficient volume or density to support an implant safely and predictably. Loss of bone can occur after long-term tooth absence, infection, or trauma, and grafting rebuilds the ridge so an implant can achieve stable anchorage. Grafting can be done at the time of extraction, as a staged procedure before implant placement, or concurrently with the implant depending on the clinical needs.
The graft material may come from the patient, a donor source, or synthetic materials chosen for their predictable healing characteristics and biological compatibility. Healing intervals vary by technique and material but typically require several months for the graft to integrate and mature. Successful grafting expands restorative options and enhances long-term implant prognosis when performed with careful surgical planning.
Implant restorations include single crowns for individual missing teeth, implant-supported bridges for adjacent missing teeth, full-arch fixed restorations that replace an entire dental arch, and implant-retained overdentures that snap onto attachments for improved retention. Each option addresses different functional and esthetic goals: single crowns preserve adjacent teeth, bridges replace multiple teeth with fewer implants, and full-arch solutions restore complete oral function for patients with extensive tooth loss. Implant-retained overdentures offer a removable solution with enhanced stability compared with conventional dentures.
The choice of restoration depends on factors such as the number and location of missing teeth, bone availability, patient preferences, and long-term maintenance considerations. Prosthetic materials and design are selected to balance strength, esthetics, and hygiene access. Collaborative planning between the surgical and restorative teams ensures the chosen restoration meets the patient’s functional and cosmetic goals.
Implants provide independent support that preserves neighboring tooth structure because they do not rely on adjacent teeth for retention, unlike traditional bridges that require preparation of healthy teeth. They also help maintain bone volume by transmitting functional forces into the jaw, reducing the resorption commonly associated with long-term denture wear. As a result, implants often offer improved chewing efficiency, greater comfort, and a more natural feel during speech and eating.
Removable dentures remain a valid option for many patients, especially when implants are not feasible or when a removable solution is preferred. However, dentures can require adjustments, adhesives, and periodic relining as the ridge changes, whereas implant-supported solutions typically offer enhanced stability and reduced day-to-day maintenance. The optimal choice depends on clinical factors, patient priorities, and the long-term plan for oral health preservation.
Long-term implant health relies on the same core practices that support natural teeth: consistent brushing, daily interdental cleaning, and regular professional examinations and hygiene visits. Special instruments such as interdental brushes or floss designed for implants can help control plaque around implant restorations, and clinicians will recommend a maintenance schedule tailored to individual risk factors. Routine surveillance includes checking soft tissue health, prosthetic fit, and radiographic monitoring when indicated.
Patients should be attentive to signs of inflammation, persistent bleeding, or mobility around an implant and seek prompt evaluation if concerns arise. Tobacco use, uncontrolled systemic conditions, and inadequate oral hygiene can increase the risk of peri-implant disease and should be addressed as part of preventive care. With proper home care and professional maintenance, implant restorations can remain functional and stable for many years.
Determining candidacy for implants begins with a comprehensive consultation that includes medical and dental history, a clinical exam, and diagnostic imaging to evaluate bone and soft tissue conditions. During this visit clinicians discuss treatment objectives, explain potential preparatory procedures, and outline the sequence of care so patients understand what to expect at each stage. Individual goals such as esthetic concerns, functional needs, and lifestyle considerations are integrated into the recommendation to arrive at a tailored plan.
The office of Erin A. Fontenot, DDS in Lafayette offers consultations and digital planning to help patients explore implant options and make informed decisions. Scheduling an evaluation is the best way to receive personalized guidance and a clear clinical assessment of suitability for implant therapy. A thoughtful, evidence-based approach ensures treatment plans prioritize long-term function, esthetics, and oral health.
