Missing teeth affect more than just your smile — they change how you eat, speak, and feel about your oral health. Implant restorations recreate the form and function of natural teeth by combining a surgically placed titanium post with a custom-crafted crown or bridge. This page explains how implant restorations work, what to expect during treatment, and how thoughtful design and upkeep help them perform reliably for many years.
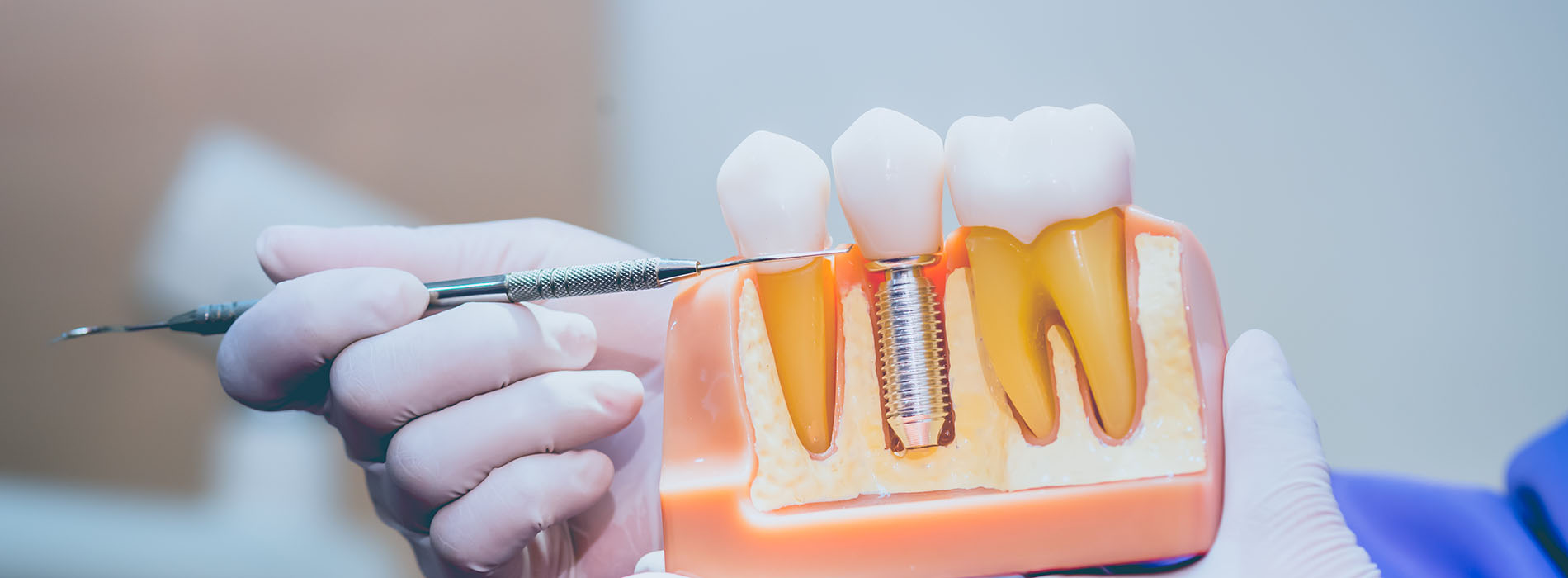
Dental implants replace the tooth root with a biocompatible post that integrates with the jawbone, creating a stable foundation for a replacement tooth. Because implants restore support beneath the gum line, they preserve surrounding bone and facial structure in a way that removable options cannot. That structural benefit translates into improved chewing efficiency and a more natural feeling when you bite and speak.
Beyond function, implant restorations are designed to look like natural teeth. Contemporary restorative materials and digital workflows allow clinicians to match color, translucency, and surface texture so crowns and bridges blend seamlessly with your smile. When planned and executed carefully, implant restorations can be indistinguishable from adjacent teeth in both appearance and performance.
Implants also avoid some of the compromises of other tooth-replacement choices. Unlike traditional bridges, implants do not require alteration of healthy neighboring teeth. And compared with removable dentures, implant-supported restorations reduce unwanted movement and offer far greater comfort for everyday activities, such as eating and speaking.
Treatment begins with a comprehensive evaluation that reviews medical and dental history, examines the mouth, and uses imaging to assess bone volume and anatomy. This planning phase determines whether a straightforward implant placement is feasible or whether supportive procedures — such as bone grafting or sinus augmentation — are recommended to create the right foundation.
Placement is typically performed in a controlled surgical setting under local anesthesia, and many patients experience minimal discomfort afterward. Once the implant is placed, the surrounding bone needs time to grow and fuse with the implant surface — a process known as osseointegration. This healing period is essential for long-term stability and can vary depending on the location and individual healing response.
After integration, an abutment connects the implant to the final restoration. At that stage our team works with the patient to finalize the shape, shade, and bite of the crown or bridge. The final prosthesis is secured to the implant system to restore full chewing function and a natural appearance, completing the transition from surgery to a finished, functional smile.
Successful implant restorations rely on careful collaboration between clinician and laboratory. Material selection is guided by the restoration's location, aesthetic demands, and functional load. Ceramic materials offer excellent color matching for front teeth, while high-strength ceramics and porcelain-fused options may be chosen for posterior restorations where durability is a priority.
Shade matching and contouring are critical to achieving a lifelike result. Digital scanning and photography allow technicians to reproduce the nuances of surrounding teeth and soft tissue, resulting in restorations that sit naturally in the smile. Proper emergence profile and contact points are also shaped to support gum health and make cleaning simpler for the patient.
Precision in occlusion — how the teeth meet — helps protect both the implant restoration and remaining natural teeth. Meticulous adjustments at the time of delivery reduce undue stress and ensure the restoration performs comfortably during everyday use. This attention to detail is part of why implant-supported crowns and bridges can provide a predictable, long-term solution.
Many adults with one or more missing teeth are candidates for implant restorations, but ideal outcomes depend on overall health and the condition of the jawbone. Factors such as smoking, uncontrolled systemic conditions, or insufficient bone height may require additional measures or tailored protocols. A detailed examination and diagnostic imaging help identify any issues that should be addressed before placing an implant.
When bone volume is limited, techniques like guided bone regeneration, grafting, or sinus lifts can rebuild adequate support. These adjunctive procedures extend implant eligibility to patients who might otherwise be unsuitable for implants and are performed with the same focus on long-term stability and patient safety.
Individualized treatment planning also considers the patient’s functional needs and aesthetic goals. Whether replacing a single tooth, supporting a multi-tooth bridge, or anchoring an overdenture, the plan balances surgical strategy, restorative design, and patient preferences so the final result is both practical and pleasing.
After placement, routine home care and professional maintenance are essential for preserving implant health. Daily brushing and flossing adapted for implant restorations remove plaque and reduce inflammation around the gum tissue. Regular dental visits allow for monitoring of the restoration, assessment of bite forces, and early detection of any complications.
Some habits — such as clenching, grinding, or biting hard objects — can place extra stress on restorations and should be discussed with your clinician. When needed, protective measures like nightguards can be provided to reduce risk. Early intervention for issues such as loosened components or changes in the surrounding gum tissue helps prevent more significant problems down the line.
When maintained properly, implant restorations offer excellent longevity. Periodic professional cleanings, radiographic checks, and clinical evaluations ensure the implant, surrounding bone, and prosthesis remain healthy and functional. Open communication with your dental team helps tailor ongoing care to your specific situation and preserves the investment in your smile.
At the office of Erin A. Fontenot, DDS, our approach to implant restorations blends modern surgical techniques with precise restorative craftsmanship to restore both form and function. If you’d like to learn more about whether implant restorations are the right solution for your smile, please contact us for additional information and to discuss next steps.
Implant restorations replace missing teeth by combining a surgically placed biocompatible post with a custom prosthesis to recreate the form and function of a natural tooth. The post acts as an artificial root that fuses with the jawbone through a process called osseointegration, providing a stable foundation for a crown, bridge or overdenture. Restorations are designed to restore chewing function, support facial structure and deliver a lifelike appearance that integrates with surrounding teeth.
Unlike removable options, implant restorations are fixed or securely anchored, which reduces movement and improves comfort during everyday activities such as speaking and eating. The restorative portion is crafted to match color, translucency and surface texture so it blends seamlessly with the smile. Careful planning and precise laboratory work ensure the final restoration performs reliably and looks natural for many years.
Implant restorations replace the tooth root as well as the visible tooth, which preserves bone volume and maintains facial support in a way removable appliances cannot. Because the implant integrates with the jaw, it prevents the bone loss that typically follows tooth extraction and helps maintain adjacent tooth stability. This structural advantage translates into improved chewing efficiency and a more natural feel when you bite and speak.
Contemporary materials and digital workflows allow clinicians to reproduce tooth color and anatomy with high precision, making implant restorations difficult to distinguish from natural teeth. Unlike traditional bridges, implants do not require reduction of healthy neighboring teeth, and compared with removable dentures they offer greater retention and comfort. Those combined benefits are why many clinicians and patients regard implants as the preferred long-term solution for tooth replacement.
Treatment begins with a comprehensive consultation that reviews medical and dental history, clinical findings and diagnostic imaging to assess bone volume and anatomy. This planning phase identifies whether the site is ready for placement or whether preparatory procedures such as grafting or a sinus augmentation are needed to create a stable foundation. A detailed plan outlines timing, prosthetic goals and any adjunctive treatments so the surgical and restorative phases align.
Implant placement is typically performed under local anesthesia in an outpatient setting, and the implant is left to integrate with the bone during a healing period. After osseointegration, an abutment is attached and impressions or digital scans are taken to finalize the shape and shade of the crown or bridge. The final prosthesis is then secured to the implant system, restoring full chewing function and completing the transition from surgery to a finished, functional smile.
Many adults who are missing one or more teeth are candidates for implant restorations, but ideal outcomes depend on overall health and the quantity and quality of the jawbone. Factors such as uncontrolled systemic conditions, smoking and certain medications can affect healing and may require modified protocols or medical clearance before treatment. A thorough clinical exam and imaging help identify any risk factors and guide individualized planning.
When bone volume is limited, techniques like guided bone regeneration, grafting or sinus lifts can rebuild support and expand eligibility for implants. These adjunctive procedures are routinely used to create the conditions necessary for predictable implant integration. Ultimately, candidacy is determined by a combination of medical status, oral anatomy and the patient’s functional and aesthetic goals, which are addressed in the treatment plan.
Restorative materials are chosen based on the restoration's location, aesthetic demands and functional load, with options including high-strength ceramics, zirconia and porcelain-fused-to-metal designs. Ceramic materials provide excellent color matching and translucency for front teeth, while denser ceramics or reinforced options may be selected for posterior teeth that endure higher biting forces. Material selection balances aesthetics and durability to meet the clinical requirements of each case.
Digital scanning, photography and collaboration with a skilled dental laboratory allow technicians to reproduce the nuances of adjacent teeth and soft tissues. Proper emergence profile and contact points are designed to support gum health and simplify home care. Precision in occlusal design and material choice helps protect the restoration and surrounding teeth from excessive wear or mechanical stress.
Daily oral hygiene is essential for maintaining implant health, including regular brushing and flossing with tools adapted for implant restorations, such as interdental brushes or floss threaders. Removing plaque and controlling inflammation around the gum tissue reduces the risk of peri-implant conditions and preserves the supporting bone. Patients should follow specific home-care recommendations provided by their clinician to protect both the restoration and surrounding tissues.
Routine professional maintenance is equally important and includes periodic cleanings, radiographic checks and clinical evaluations to monitor bone levels and restoration integrity. The dental team can detect early signs of complications, assess occlusion and make necessary adjustments to minimize stress on the implant. When habits such as grinding or clenching are present, protective measures like a nightguard can be recommended to reduce risk and extend the restoration's lifespan.
While implant restorations have high success rates, potential risks include infection around the implant (peri-implant mucositis or peri-implantitis), mechanical issues such as loose components or fracture, and complications related to surgical placement. Many risks are reduced through careful planning, aseptic technique and proper patient selection, but early recognition is important when problems arise. Regular follow-up visits help identify changes in tissue health, bone levels or prosthetic fit before they escalate.
Management of complications depends on the cause and severity, ranging from improved hygiene and non-surgical therapy to surgical intervention or component repair. Mechanical problems can often be resolved by replacing or tightening parts, while biological issues may require debridement, antibiotics or regenerative procedures. Open communication with the dental team ensures timely treatment and preserves the long-term stability of the restoration.
Implant restorations can last many years or decades when supported by good oral hygiene, regular professional care and favorable medical conditions. Longevity is influenced by factors such as the patient’s systemic health, smoking status, quality of the supporting bone, material selection and the precision of the restorative work. Proper occlusal management and avoidance of excessive forces also play a major role in preserving both the implant and the prosthesis.
Routine monitoring with clinical exams and radiographs allows early intervention for issues that might shorten lifespan, while professional cleanings help control plaque and inflammation. Addressing parafunctional habits, maintaining stable periodontal health and following the clinician’s maintenance schedule are practical steps patients can take to protect their investment. With attentive care, many patients experience long-term function and satisfaction from their implant restorations.
Implant placement is typically performed in an outpatient setting under local anesthesia and sometimes sedation, depending on the patient’s needs and the complexity of the case. Many patients experience minimal discomfort during the procedure, and common post-operative symptoms include mild swelling, light bleeding and tenderness that can be managed with prescribed or over-the-counter medications and cold compresses. Clear post-operative instructions help promote uneventful healing and reduce the risk of complications.
The initial healing period focuses on soft tissue recovery and the longer process of osseointegration, during which the implant becomes firmly anchored in the bone. Healing times vary by individual and by implant location, and the clinician will schedule follow-up visits to assess progress and determine when the restorative phase can proceed. Patients are typically advised to follow a modified diet and maintain careful oral hygiene during the early recovery phase to support predictable outcomes.
Our approach blends modern surgical techniques with precise restorative craftsmanship to restore both form and function while emphasizing whole-body wellness and patient comfort. Treatment begins with a thorough evaluation and diagnostic imaging to create an individualized plan that addresses bone anatomy, aesthetic goals and long-term stability. The team coordinates closely with dental laboratories and specialists when needed to ensure the prosthesis matches adjacent teeth in color, contour and function.
Throughout treatment we prioritize clear communication, predictable protocols and attentive follow-up care to monitor implant health and prosthetic performance. Patients receive personalized home-care guidance and scheduled maintenance to protect the implant and surrounding tissues. If you would like to discuss whether implant restorations are the right option for your smile, please contact the office to arrange a consultation.
