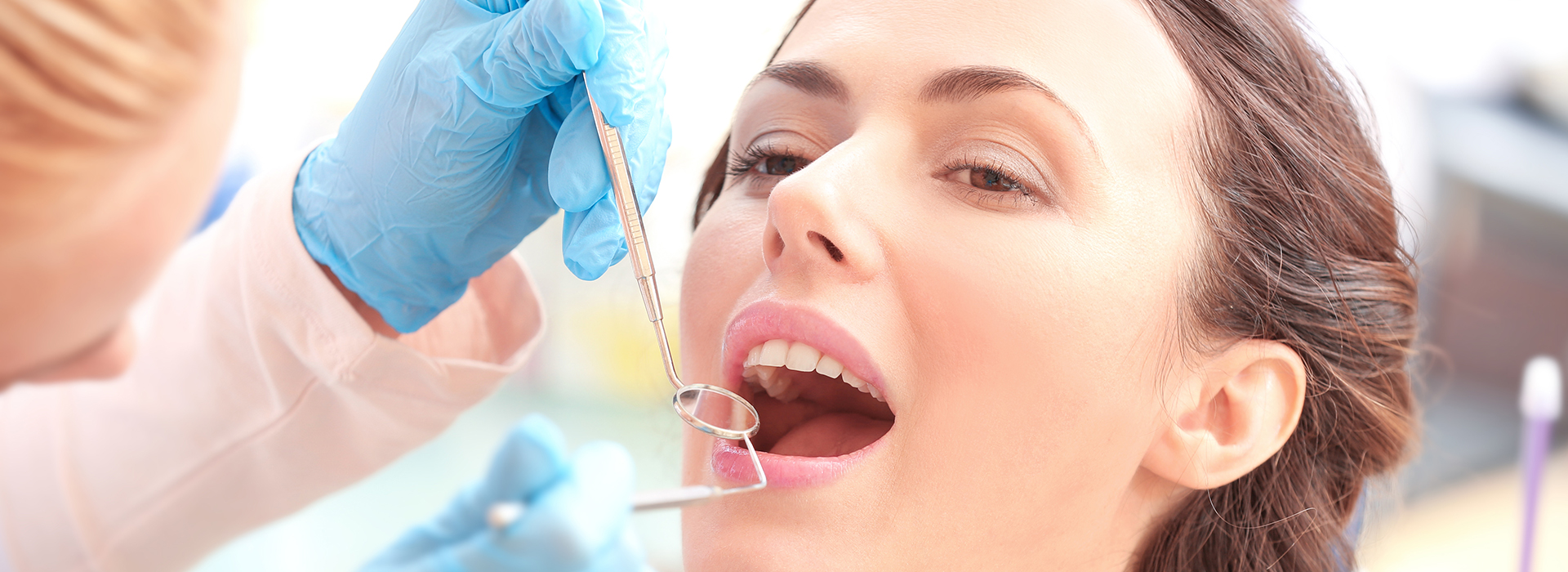
Gum disease is the leading cause of adult tooth loss and yet it often develops quietly. Public health data show that nearly half of adults over 30 have some form of periodontal disease, and many people don't realize symptoms can be subtle at first. At the office of Erin A. Fontenot, DDS, we provide focused periodontal care designed to preserve your natural teeth, protect your overall health, and help you enjoy a comfortable, functional smile for years to come.
Periodontal disease starts when bacterial biofilm (plaque) accumulates along the gumline and beneath the gums. Over time this bacterial presence triggers inflammation in the tissues that surround and support the teeth — the periodontium — which includes the gum tissue, periodontal ligament, and the jawbone. If not addressed, that inflammation can progress and produce structural changes that reduce tooth stability.
Early stages are typically limited to the soft tissues and are reversible with improved oral hygiene and professional care. Left unchecked, however, chronic inflammation can lead to irreversible damage to the connective tissues and bone that anchor teeth. Understanding this progression helps patients and clinicians intervene earlier and more effectively.
Because periodontal conditions often develop without pain, routine dental examinations and periodontal assessments are essential. Regular monitoring allows clinicians to catch small problems before they become major issues and to tailor prevention and treatment plans to each person's needs.
Common signs that warrant an evaluation include:
Red, swollen, or tender gums
Bleeding during brushing or flossing
Receding gumlines or newly exposed tooth roots
Sensitivity to hot and cold or an ongoing bad taste or breath
Loose teeth, changes in how teeth meet, or gaps developing between teeth

Oral health and overall health are closely linked. Chronic periodontal inflammation has been associated with systemic conditions such as diabetes, cardiovascular disease, and certain respiratory issues. While the exact relationships vary by condition and individual, controlling gum inflammation reduces oral infection risk and can lower inflammatory burden on the body.
Good periodontal health supports nutrition, speech, and quality of life. When gum tissue and bone are stable, chewing is more efficient, denture fit is more predictable, and restorative options (like implants) have a more predictable foundation. Maintaining periodontal health is therefore an important part of whole-body wellness and long-term dental planning.
Prevention and early treatment are the most reliable ways to protect those broader health benefits. This means combining consistent home care with professional periodontal evaluations and individualized maintenance schedules to keep inflammation under control.
At the office of Erin A. Fontenot, DDS, we utilize advanced clinical testing through OralDNA® Labs to provide a deeper understanding of your oral health. OralDNA® Labs is a leader in salivary diagnostics, offering reliable, science-driven testing that helps detect and assess disease at earlier, more manageable stages. This allows us to move beyond surface-level evaluations and deliver more precise, proactive care.
By incorporating OralDNA® testing into our approach, we are able to identify harmful bacteria, screen for oral HPV, and develop highly personalized treatment plans. This level of insight helps us improve outcomes, reduce long-term risks, and support your health with greater accuracy and confidence.
The OralDNA® test is simple, comfortable, and non-invasive. During your visit, you will rinse with a sterile saline solution to collect bacteria from throughout your mouth and then provide a small saliva sample in a collection tube. The sample is carefully sealed and sent to a certified laboratory for advanced molecular analysis. There are no needles, no discomfort, and the entire process takes only a few minutes. Once your results are returned, we will review them with you in detail so you gain a clear understanding of which bacteria are present, what they mean for your oral and overall health, and how your treatment plan will be tailored moving forward.
Gingivitis is the earliest, reversible stage of gum disease. It typically presents as gum redness, mild swelling, and bleeding during oral hygiene routines. Many people discover gingivitis after noticing blood on their toothbrush or when their gums feel more tender than usual.
Because gingivitis does not damage the supporting bone, prompt treatment and improved cleaning techniques usually restore healthy tissue. Professional scaling to remove plaque and tartar, combined with targeted oral hygiene instruction, commonly reverses the inflammation and prevents progression.
Responding quickly is the key: with consistent care and follow-up, patients can often avoid more invasive treatments. Annual or semi-annual periodontal checks make it easier to document improvement and confirm that home care and professional treatments are effective.

If gingivitis is not corrected, the condition can advance to periodontitis, in which the infection extends deeper and begins to compromise the soft tissue attachments and supporting bone. Clinically this often shows as deeper pockets between teeth and gums, gum recession, and, in some cases, mobility of the teeth.
Periodontitis is staged by how much tissue and bone have been lost and by how rapidly the condition is progressing. Treatment goals shift from simply reversing inflammation to stabilizing the disease, preserving existing support, and, when possible, regenerating lost tissue. That process requires a thorough diagnosis and a customized treatment plan.
Modern periodontal care offers a spectrum of approaches aimed at controlling infection, reducing pocket depths, and restoring a healthy environment for the teeth. When appropriate, regenerative techniques and grafting can improve structural support and prepare sites for future restorative work.
The health of your mouth is closely connected to the health of your entire body. Research has shown that oral bacteria can contribute to serious conditions such as heart disease, diabetes, stroke, and complications during pregnancy. OralDNA® testing allows us to identify the specific bacteria associated with periodontal disease and evaluate how they may be impacting both your oral condition and your overall health.
When harmful bacteria are present at elevated levels — especially in combination with an individual's inflammatory response — they can lead to symptoms such as bleeding gums, bone loss, and eventual tooth loss. Over time, these same bacteria may also increase the risk of broader health concerns, making early detection and management essential.
As an authorized Perio Protect provider, we are able to offer patients a clinically proven, non-invasive way to manage gum disease between professional visits. Perio Protect uses customized prescription trays — similar in appearance to a thin mouth guard — that are precisely fitted to each patient's unique anatomy. These trays are designed with a specially engineered seal that delivers medication deep into the periodontal pockets where harmful bacteria live, an area that brushing, flossing, and even traditional rinses cannot reliably reach.
The trays are worn at home for short intervals each day, typically just minutes at a time, making them easy to incorporate into a daily routine. The medication used — most commonly a low-concentration hydrogen peroxide gel — works to disrupt the bacterial biofilm that drives gum disease, reducing inflammation and helping the gums heal over time. Many patients notice improvements such as reduced bleeding, fresher breath, and healthier-looking gum tissue as treatment progresses.
Perio Protect is not a replacement for professional periodontal care — it is a powerful complement to it. By targeting bacteria in the pockets on a daily basis, the trays help slow recolonization between cleanings and support the results achieved through in-office scaling and root planing. For patients managing active periodontal disease or those who are prone to recurring gum inflammation, Perio Protect trays can play a meaningful role in achieving and maintaining long-term stability.
If you are a candidate for Perio Protect, we will take precise impressions to fabricate your custom trays and provide clear instructions on how and when to use them. We will also monitor your progress at follow-up visits and adjust your protocol as your gum health improves.
At the office of Erin A. Fontenot, DDS, we focus on creating individualized periodontal plans that reflect each patient's health, lifestyle, and goals. Our approach begins with a comprehensive evaluation that includes periodontal charting, radiographic review, and an assessment of risk factors such as smoking, systemic disease, or genetic predisposition.
From there, we recommend the least invasive, evidence-based measures that are likely to achieve lasting health — whether that is enhanced home care and non-surgical therapy or, when necessary, more advanced interventions. Our aim is to halt disease progression and, wherever possible, restore form and function to the supporting tissues.
We also emphasize ongoing maintenance: periodontal health is not a one-time achievement but a partnership between clinician and patient. Regular periodontal cleanings and examinations are essential to sustain the improvements gained through initial therapy.
Treatment is tailored to the stage of disease and the individual's clinical findings. Early, localized inflammation can often be managed with professional scaling, improved daily oral hygiene, and short-term antimicrobial measures. More advanced disease requires a broader treatment plan aimed at eliminating bacterial reservoirs and reestablishing healthy tissue contours.
We discuss each step with patients so they understand the rationale for care, realistic outcomes, and the maintenance required to preserve results. Managing periodontal disease often involves a sequence of visits — initial therapy, reassessment, and then either continued non-surgical maintenance or referral to specialized surgical care if needed.
Open communication and patient education are central to lasting success. We encourage questions and provide clear guidance on home care tools and techniques that make a real difference in healing and long-term stability.
When detected early, periodontal disease can often be controlled with conservative measures. Scaling and root planing remove plaque and hardened deposits that lie below the gumline and smooth root surfaces to help tissues reattach. Adjunctive topical or systemic antimicrobials may be used in specific cases to reduce bacterial load.
These techniques aim to stop inflammation, decrease pocket depths, and restore gingival health without incisions. With an effective home-care routine and regular professional maintenance, many patients maintain long-term stability after non-surgical therapy.
When conservative care does not achieve the desired improvement, we reassess and consider additional options to control the disease and protect tooth support.
For more advanced periodontitis, surgical approaches can access deep pockets, remove diseased tissue, and reshape supporting bone to reduce pocket depth. Common surgical goals include eliminating bacterial reservoirs and creating anatomy that is easier to keep clean.
Regenerative techniques — such as bone grafts, guided tissue regeneration, and soft tissue grafts — are used when appropriate to rebuild lost structure, improve aesthetics, and provide better support for teeth or restorative solutions like implants.
Contemporary periodontal surgery is performed with an emphasis on patient comfort, precision, and predictable outcomes; technologies such as laser therapy may also play a role when clinically indicated.
Eliminate subgingival bacterial deposits from root surfaces
Stabilize and, where possible, rebuild bone and soft tissue support
Reduce pocket depth to make daily cleaning more effective and maintain periodontal health
Summing up, periodontal care is a vital component of preserving your natural teeth and protecting your overall health. If you have noticed bleeding gums, increased sensitivity, or any changes in how your teeth feel, please contact us to learn more about evaluation and treatment options. Our team is available to answer questions and help you take the next step toward lasting periodontal health.
Most people don’t realize that periodontal disease is the leading cause of tooth loss among adults. According to statistics from the Centers for Disease Control and Prevention, one out of every two adults over the age of 30 in the United States has periodontal disease.
You may be surprised to learn that the human mouth is home to a wide variety of microbes. The fact is that over 700 different strains of bacteria have been detected in the oral cavity. Although some of these bacteria are beneficial, others are harmful to oral health. Without proper oral hygiene and routine dental care, these harmful bacteria can cause tooth decay and gum disease, compromising both your oral health and overall wellbeing.
In addition to inadequate oral hygiene and infrequent professional care, other factors, including smoking, genetic tendencies, and unchecked diabetes, can contribute to the escalation of periodontal disease.
Your gums and teeth have an interdependent relationship, which means healthy teeth depend on the support of healthy gums. Also, taking care of your smile does more than keep your teeth and gums in optimal condition; good oral health also supports systemic health. In addition to being the leading cause of tooth loss in adults, researchers are finding more and more links between periodontal disease and a number of medical problems, including heart disease, stroke, diabetes, respiratory problems, and adverse pregnancy outcomes such as pre-term and low birth-weight babies.
If you notice that your gums are bleeding with the slightest pressure while brushing or flossing, it’s a sign of gingivitis. Although gingivitis is the earliest stage of gum disease, it can easily be reversed with deeper cleanings as well as an improved regimen of oral hygiene at home.
In the absence of professional treatment and better home care, gingivitis progresses to the next stage, which is known as periodontitis. In this stage, the connective tissue and bone that hold the teeth in place begin to break down with an increase in pocketing between the teeth and bone, gum recession, and bone loss. Without proper treatment by your dentist, periodontitis will progress from a mild to moderate loss of supporting tissue to the destruction of the bone around the teeth.
Although gingivitis can often be reversed with improved oral hygiene and professional cleanings, as periodontal disease advances, more extensive procedures are required to halt its progression. Based on a complete assessment of your periodontal health and a review of possible contributing factors, our office will recommend the best options in care. Treatment for periodontitis may include a series of deeper cleanings known as root planing and scaling, surgical procedures to reduce pocket depth, bone or tissue grafts, laser procedures, or antimicrobial medications.
The cost of care depends on the type of procedures required to restore your periodontal health. If you have dental insurance, plans often cover treatment to prevent gum disease as well as many procedures to treat the various stages of gum disease. Our goal is to help patients restore and maintain good oral health. We do all we can to help you begin care without additional stress or delay. Our business office works with you to maximize your benefits and provide easier, more convenient payment options.
By seeing our office regularly for care and doing your best to eat a healthy diet and practice good oral hygiene, you can keep your smile in tip-top shape as well as protect your overall wellbeing.
At the office of Erin A. Fontenot, DDS, we provide a comprehensive range of services to address all your oral healthcare needs. You can rest assured that your smile is in the best of hands at our office. Our skilled and experienced team maintains a position at the forefront of advances in care and remains dedicated to providing the highest quality of skilled and compassionate treatment.
Periodontal disease begins when bacterial biofilm, commonly called plaque, accumulates along the gumline and beneath the gums. This bacterial presence provokes an inflammatory response in the periodontium, the tissues that support your teeth, which includes the gum tissue, periodontal ligament and underlying bone. Over time, persistent inflammation can lead to destruction of these supporting structures and increased tooth mobility.
Risk factors such as smoking, poorly controlled systemic conditions like diabetes, certain medications, and genetic susceptibility increase the likelihood that plaque will trigger progressive disease. Changes in hormones, stress, and inadequate oral hygiene also affect how aggressively the tissues respond to bacterial challenge. Identifying and addressing these contributors helps clinicians create an effective prevention and treatment plan.
Early periodontal disease, or gingivitis, most often shows up as red, swollen or tender gums and bleeding during brushing or flossing. Some patients notice persistent bad breath or a bad taste in the mouth as an early symptom, while others discover gum changes only during a dental visit. Because early stages usually do not cause pain, many people miss these warning signs without routine exams.
Catching gingivitis early is important because the condition is reversible with professional care and improved home hygiene. Regular periodontal assessments allow clinicians to monitor pocket depths and tissue health so that small problems can be managed before they progress. If you notice any of these changes, scheduling an evaluation helps prevent more invasive treatment later.
Diagnosis begins with a comprehensive clinical exam that includes periodontal charting to measure pocket depths, assessment of gum recession and tooth mobility, and evaluation of bleeding on probing. Radiographs are used to assess bone levels and detect any underlying bone loss that may not be visible during a visual exam. A thorough medical history and review of risk factors such as smoking or systemic disease are also part of the evaluation.
Clinicians combine these findings to determine the stage and grade of disease, which guides treatment planning and follow-up frequency. In some cases, microbial testing or referral to a specialist may be recommended to refine therapy. Accurate diagnosis helps ensure care is matched to the patient’s clinical needs and long-term goals.
Conservative, non-surgical therapy typically begins with professional scaling and root planing to remove plaque and hardened deposits from below the gumline and to smooth root surfaces. This procedure reduces bacterial reservoirs and helps inflamed tissues reattach to the tooth surface, often combined with targeted antimicrobial measures when clinically indicated. Improved home care and patient education are essential components to reinforce the benefits of professional treatment.
After initial therapy, the clinician reassesses healing and pocket depths to determine whether further treatment is needed or if the patient can transition to regular maintenance. Many patients achieve long-term stability with effective non-surgical care plus consistent periodontal maintenance appointments. When non-surgical measures do not deliver the necessary improvement, the care team will discuss additional options.
Scaling and root planing is performed to remove subgingival plaque and calculus and to create a clean, smooth root surface that supports tissue healing. The procedure is usually done under local anesthesia for comfort and may be completed over one or more visits depending on the extent of disease. Patients commonly experience some sensitivity or mild tenderness afterward, which typically resolves as healing progresses.
Following therapy, clinicians provide guidance on home care techniques and may recommend short-term antimicrobial rinses or localized medications to support recovery. A re-evaluation is scheduled several weeks after treatment to measure pocket reduction and determine whether additional care is necessary. Successful outcomes rely on both professional therapy and the patient’s ongoing oral hygiene efforts.
Surgical intervention is considered when non-surgical therapy cannot adequately reduce deep periodontal pockets or when anatomic factors prevent effective cleaning and maintenance. Surgery allows clinicians to access deep disease sites, remove diseased tissue, reshape bone if needed, and reduce pocket depths to make daily home care more effective. In cases of significant tissue or bone loss, regenerative procedures such as bone grafts or guided tissue regeneration may be recommended to rebuild support.
The decision to pursue surgery is based on a thorough reassessment and a discussion of realistic goals, potential benefits and expected maintenance. Contemporary periodontal surgery emphasizes patient comfort, minimally invasive techniques when possible, and predictable outcomes. If surgical care is recommended, the practice will explain each step and coordinate follow-up to monitor healing and long-term stability.
Yes. Chronic periodontal inflammation contributes to the body’s overall inflammatory burden and has been associated with systemic conditions such as diabetes and cardiovascular disease. While the exact nature of these relationships varies by individual and condition, controlling periodontal infection reduces oral inflammation and can improve markers of systemic health in many patients. Maintaining healthy gums also supports nutrition, speech and quality of life.
Because of these links, clinicians take a whole-body approach to periodontal care, considering medical history and coordinating with other healthcare providers when appropriate. Patients with systemic conditions often benefit from more frequent monitoring and personalized periodontal maintenance to help protect both oral and overall health. Open communication about medical history and medications enables better clinical decisions.
Consistent, effective home care is the foundation of periodontal health and complements professional treatment. Recommended steps include brushing twice daily with a soft-bristled brush, daily interdental cleaning with floss or interdental brushes, and using any adjuncts your clinician prescribes such as antimicrobial rinses or specialized tools. Technique matters as much as frequency, so follow the specific guidance provided during your appointment.
After in-office therapy, clinicians may suggest short-term changes to reduce sensitivity and support healing, along with a personalized maintenance schedule. Patients should promptly report persistent bleeding, pain or changes in tooth fit, since early re-evaluation helps prevent recurrence. Long-term success depends on the partnership between patient diligence and regular professional care.
Periodontal maintenance consists of professionally performed cleanings and assessments focused on removing subgingival deposits, monitoring pocket depths and reinforcing home care techniques. The frequency of maintenance visits is individualized based on disease severity, response to therapy, and risk factors, and it commonly ranges from every three to six months. These visits are essential to sustain improvements gained through initial treatment and to detect any early signs of recurrence.
During maintenance appointments, clinicians reassess clinical measurements and may take updated radiographs when indicated to track bone levels. Adjustments to maintenance frequency or additional therapy are made if disease activity is detected. Patients who adhere to a recommended maintenance schedule significantly reduce their risk of progressive periodontal loss.
At the office of Erin A. Fontenot, DDS we begin with a comprehensive evaluation that includes periodontal charting, radiographic review and discussion of medical history and lifestyle factors to identify individual risk contributors. Treatment plans are tailored to each patient’s clinical findings and goals, prioritizing the least invasive, evidence-based measures likely to achieve lasting health. Patient education and shared decision-making are central so individuals understand the rationale and expected outcomes of their care.
When advanced therapy is needed, we coordinate referrals or combine regenerative and surgical approaches as appropriate to restore support and prepare sites for future restorative work. Ongoing maintenance and clear home-care instructions are emphasized to protect long-term results. Our team remains available to answer questions and adjust care as a patient’s needs evolve.
