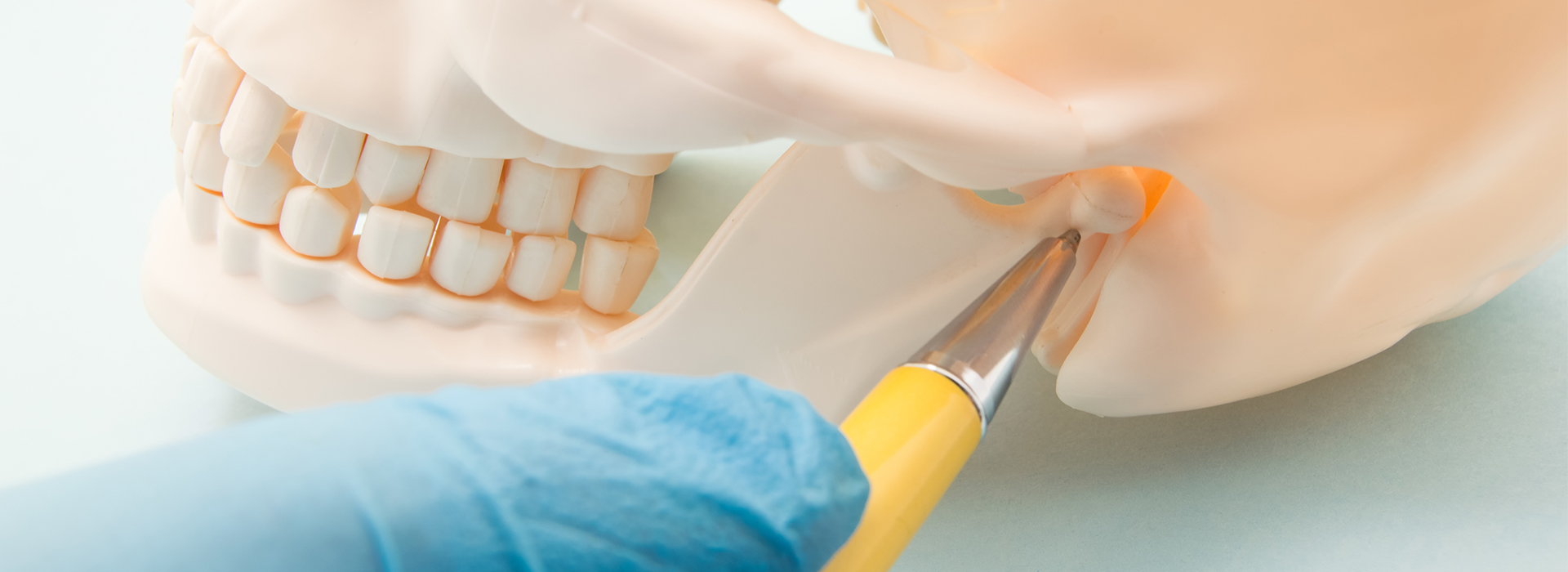
The temporomandibular joint (TMJ) is a small but remarkably complex structure that connects the lower jaw to the skull. It allows the jaw to hinge open and closed, glide forward and back, and move side to side—motions we rely on for speaking, chewing, and facial expression. Within each joint sits a soft, shock-absorbing disc that helps the bony surfaces glide smoothly and protects the joint during everyday forces.
Because the TMJ must perform both hinge and sliding actions in a tight space, it depends on precise coordination among bones, muscles, ligaments, and nerves. Even subtle changes in how the teeth meet, how the muscles work, or how the disc moves can alter that balance and give rise to symptoms. That combination of multiple moving parts is why TMJ problems can feel complex and elusive to diagnose.
Understanding the joint’s anatomy helps explain why TMJ disorders can affect more than just the jaw. Nearby structures—ears, neck muscles, and nerves—are all influenced by the jaw’s position and movement. When the TMJ is out of sync, people may experience pain patterns or functional limitations that extend beyond the joint itself.
TMJ problems can develop from a range of forces and conditions. One frequent contributor is repetitive stress on the joint, often caused by clenching or grinding the teeth (bruxism). These habits place persistent pressure on the joint and surrounding muscles, gradually wearing tissues and provoking inflammation. Acute trauma, such as a blow to the jaw or a sudden forceful movement, can also damage the disc or the joint surfaces.
Arthritic changes are another important factor. Degenerative conditions like osteoarthritis or inflammatory types such as rheumatoid arthritis can affect the TMJ’s cartilage and bone, producing pain and reduced mobility. Additionally, bite differences, prior dental work, and the position of the teeth can change how force is transmitted through the jaw and increase the risk of dysfunction over time.
Beyond mechanical causes, lifestyle and systemic factors matter. Chronic stress can increase muscle tension in the face and neck, hormonal differences may influence pain perception, and certain medical conditions can make joints more vulnerable. For many people, TMJ disorders result from a combination of triggers rather than a single identifiable cause.
Symptoms of TMJ disorders vary widely from person to person. Some people notice aching jaw pain that worsens with chewing, while others experience stiffness, catching, or a sensation that the jaw doesn’t move smoothly. Audible noises such as popping, clicking, or grinding when opening or closing the mouth are common and may indicate disc displacement or altered joint mechanics.
TMJ-related discomfort often appears alongside other complaints that might not immediately be linked to the jaw. Headaches, ear-related sensations like fullness or ringing, neck and shoulder pain, and facial muscle fatigue are frequently reported. Because symptoms can overlap with dental, neurological, and ear-nose-throat conditions, a careful clinical evaluation is important to identify the TMJ as the source.
The intensity and duration of symptoms also differ. For some, an episode of pain resolves with short-term self-care; for others, symptoms persist or flare intermittently and can affect sleep, eating, and daily activities. Recognizing patterns—what makes symptoms better or worse—helps guide an effective treatment approach.
A comprehensive assessment begins with a detailed clinical interview and a hands-on examination. A practitioner will ask about symptom history, jaw habits, dental work, prior injuries, and any related health issues. During the exam, the clinician evaluates jaw range of motion, listens for joint sounds, palpates muscles for tenderness, and observes how the teeth come together. These findings help distinguish muscle-related pain from true joint pathology.
Imaging and targeted tests may be used to clarify the underlying cause when the clinical picture is unclear or when conservative care has not produced expected improvement. Panoramic X-rays, cone-beam CT scans, or MRI can reveal bony changes, disc position, or soft-tissue inflammation. In some cases, referral to a specialist such as an oral and maxillofacial surgeon, a pain specialist, or a physical therapist is recommended to refine diagnosis and coordinate care.
Because TMJ disorders can intersect with dental occlusion and facial muscle function, a collaborative approach often yields the best results. Your dental team can evaluate bite relationships and how restorative or orthodontic treatments might influence joint health, while allied health professionals can address posture, muscle balance, and central pain mechanisms.
The majority of TMJ problems respond well to conservative, reversible treatments focused on reducing pain and restoring function. At-home strategies—short-term soft diets, avoiding extreme jaw movements, applying cold or warm packs, and practicing relaxation or biofeedback techniques—can ease symptoms for many people. Over-the-counter anti-inflammatory medications may be helpful when used as directed under clinical guidance.
When additional intervention is needed, oral appliances such as custom night guards or stabilization splints are commonly used to reduce grinding and redistribute forces across the teeth and joints. Physical therapy, including hands-on soft-tissue work, jaw exercises, and posture training, complements appliance therapy by improving muscle coordination and joint mobility. For targeted relief, minimally invasive treatments such as corticosteroid or hyaluronic acid injections may be considered in select cases.
Occlusal adjustments, orthodontics, or prosthodontic care can be part of a treatment plan when bite relationships significantly contribute to symptoms, and surgical options are reserved for persistent, severe cases with clear structural abnormalities. Throughout care, the emphasis is on individualized, evidence-informed strategies that minimize risk and prioritize measurable improvement in function and comfort. The office of Erin A. Fontenot, DDS follows a measured approach, coordinating with specialists when advanced diagnostics or interventions are appropriate.
In summary, TMJ disorders arise from a mix of mechanical, inflammatory, and behavioral factors and can present with varied symptoms that extend beyond the jaw. A careful evaluation and stepwise treatment plan—starting with conservative care and progressing to targeted therapies when necessary—offer the best pathway to relief and restored function. If you would like to learn more about TMJ disorders or discuss how they are evaluated and treated in our practice, please contact us for additional information.
The temporomandibular joint, or TMJ, is the hinge that connects your lower jaw to the skull and allows chewing, speaking, and facial expression. A TMJ disorder refers to pain or dysfunction arising from the joint itself, the cushioning disc inside the joint, or the surrounding muscles and ligaments. These disorders can range from intermittent discomfort to persistent limitations in jaw movement.
Because the TMJ performs both hinge and sliding motions in a compact space, even small changes in joint mechanics or muscle coordination can produce symptoms. Disc displacement, muscle tension, and inflammation are common contributors to dysfunction. Evaluating the specific source of symptoms is essential for choosing an effective treatment plan.
Common signs of a TMJ disorder include jaw pain or tenderness, difficulty opening or closing the mouth fully, and audible noises such as clicking, popping, or grinding when moving the jaw. Some people also experience a sensation of the jaw catching or locking during movement. Symptoms often worsen with chewing, yawning, or prolonged oral activity.
TMJ-related problems frequently occur alongside other complaints like headaches, ear fullness or ringing, and neck or shoulder pain, which can make diagnosis challenging. The pattern, timing, and triggers of symptoms help clinicians distinguish TMJ disorders from dental, ear, or neurological conditions. Documenting what makes symptoms better or worse is a useful step before evaluation.
TMJ disorders are usually multifactorial, often resulting from a combination of mechanical stresses, muscle hyperactivity, and inflammatory or degenerative changes. Repetitive habits such as clenching or grinding the teeth (bruxism), acute trauma to the jaw, and long-term overload can wear joint tissues and provoke pain. Degenerative conditions like osteoarthritis or inflammatory arthritis may also affect the joint surfaces and reduce mobility.
In addition to mechanical factors, systemic and behavioral influences play a role; stress-related muscle tension, sleep disturbances, and certain medical conditions can increase susceptibility. Bite relationships and prior dental work may change how forces pass through the jaw and sometimes contribute to dysfunction. For most patients, several interacting factors explain the onset and persistence of symptoms.
A thorough evaluation starts with a detailed history and hands-on clinical examination that assesses jaw range of motion, joint sounds, muscle tenderness, and how the teeth meet. The clinician will ask about symptom patterns, oral habits, prior injuries, and any related medical issues to narrow potential causes. Exam findings help differentiate muscle-based pain from true joint pathology and guide whether imaging is needed.
When the diagnosis is unclear or symptoms persist despite conservative care, targeted imaging such as panoramic X-rays, cone-beam CT, or magnetic resonance imaging (MRI) can clarify disc position, bony changes, or soft-tissue inflammation. In selected cases, consultation with specialists in oral and maxillofacial surgery, pain management, or physical therapy improves diagnostic accuracy and care coordination. A collaborative approach often yields the best outcomes for complex cases.
Most TMJ problems respond well to conservative, reversible therapies that focus on pain reduction and restoring function. Initial strategies commonly include a short-term soft diet, avoiding wide or repetitive jaw movements, applying heat or cold, and practicing relaxation techniques to reduce muscle tension. Over-the-counter anti-inflammatory medications may provide temporary relief when used as directed under clinical guidance.
Physical therapy that incorporates jaw exercises, manual soft-tissue techniques, and posture training can improve muscle coordination and joint mobility. Custom oral appliances, behavioral modification for grinding or clenching, and a structured home-care plan are often combined to maximize improvement. The goal of conservative care is measurable symptom relief with minimal risk, progressing only to more invasive options if necessary.
Oral appliances are commonly recommended when tooth grinding or clenching places excessive stress on the joint and surrounding muscles, or when bite-related forces appear to contribute to symptoms. A stabilization splint or night guard redistributes occlusal forces, reduces muscle activity during sleep, and can protect teeth from wear. These devices are typically custom-made and adjusted over time to optimize comfort and function.
Appliance therapy is most effective when paired with other measures such as physical therapy, behavioral strategies, and addressing contributing medical factors. Regular follow-up is important to monitor symptom response and make necessary adjustments. If an appliance does not provide adequate relief, the treatment plan is reassessed and refined in collaboration with the patient.
Stress commonly increases facial and jaw muscle tension, which can lead to habitual clenching and teeth grinding (bruxism) that overload the TMJ. Repeated cycles of excessive force damage soft tissues, increase inflammation, and perpetuate pain, creating a cycle that maintains or worsens symptoms. Sleep-related bruxism in particular can be a significant and unrecognized contributor to TMJ problems.
Behavioral strategies such as relaxation training, sleep hygiene, and biofeedback can reduce daytime clenching and improve symptom control. When indicated, oral appliances combined with targeted therapies address the mechanical consequences of bruxism. A comprehensive plan that includes both behavioral and physical interventions tends to produce the best long-term results.
Yes. TMJ disorders often produce referred pain that can present as tension-type headaches, temple pain, or pain that seems to originate in the ear. Patients may report ear fullness, popping, or ringing even though the ear structures themselves are normal, since the TMJ and middle ear are anatomically close and share nerve pathways. Differentiating TMJ-related ear sensations from primary ear conditions is a common diagnostic task.
Evaluation may include an assessment by an ear-nose-throat clinician to rule out primary otologic disease when ear symptoms are prominent. Treating the underlying TMJ problem with physical therapy, appliance therapy, and behavioral modification frequently reduces associated headaches and ear complaints. Multidisciplinary care ensures that other potential causes are considered and managed appropriately.
Surgery is reserved for a minority of patients whose TMJ dysfunction has a clear structural cause and who have not improved with comprehensive conservative care. Indications may include persistent mechanical derangement, significant joint degeneration, or internal derangements that impair function and quality of life. Surgical options range from minimally invasive arthroscopy to open joint procedures, and selection depends on the specific pathology and goals of care.
Because outcomes vary and risks exist, careful evaluation by a specialist in TMJ surgery is essential before proceeding, and non-surgical options are generally exhausted first. Preoperative planning, informed consent, and coordination with the dental team and other specialists help set realistic expectations. When appropriate, surgery can restore function, but it is considered only after a measured trial of reversible therapies.
Our evaluation begins with a detailed review of your symptoms, dental history, and any prior treatments, followed by a hands-on examination of jaw motion, joint sounds, and muscle tenderness. Imaging is ordered only when clinically indicated to clarify joint structure or disc position, and we coordinate with physical therapists or medical specialists when a multidisciplinary approach will benefit the patient. The emphasis is on identifying modifiable contributors and creating a stepwise management plan focused on conservative, reversible care.
The office of Erin A. Fontenot, DDS works to provide individualized treatment plans that combine home-care strategies, appliance therapy when appropriate, and referrals to allied professionals as needed. Regular follow-up allows us to track progress and adjust therapy to achieve lasting improvements in comfort and function. If you are experiencing TMJ symptoms, scheduling an evaluation is the best first step toward a personalized plan of care.
